Head and neck
Vol. 46: Issue 2 - April 2026
Survival and prognostic factors of parotid malignancies in Northern Italy: a multicentric study
Summary
Objective. The aim of this study is to report oncological outcomes of a multicentric cohort of surgically- treated parotid gland malignancies (PGMs) and compare them with other Italian Institutions.
Methods. This is a retrospective multicentric study on surgically-treated patients with PGM. Overall survival (OS), disease-free survival (DFS) and disease-specific survival (DSS) at 5 years were calculated. The Cox proportional hazard model was used for uni- and multivariate analyses. A qualitative review of the Italian literature was performed.
Results. One-hundred and six patients were included. Negative prognostic factors included deep lobe involvement, size > 4 cm, advanced stage, margin status, histological grade, nodal involvement and extranodal disease. Parotidectomy extent did not influence DSS or DFS for T1-T2 superficial tumours. The occult lymph node metastasis rate was 30.8%. Neither elective neck dissection (END) nor elective neck irradiation (ENI) influenced DFS or DSS.
Conclusions. Deep lobe removal in pT1-T2 superficial tumours may not always be necessary. END and ENI did not show a significant impact on prognosis, despite a high incidence of occult nodal metastasis. Further studies are needed to fully evaluate the impact of these therapeutic options in subgroups of patients with PGMs.
Introduction
Salivary gland tumours represent around 1-3% of head and neck tumours and 0.3% of all malignant tumours. They more frequently involve males, with a male to female ratio of 1.3:1 and the higher incidence of cases is usually found during the fifth to sixth decade of life. Most salivary gland malignancies (around 70%) occur in the parotid gland, the most common being mucoepidermoid carcinoma (MEC), followed by acinic cell carcinoma (AciCC) and adenoid cystic carcinoma (ACC).
Low incidence combined with histological heterogeneity and unpredictable behaviour pose a challenge in the diagnostic work-up, treatment strategy and prognostication of oncological outcomes of parotid gland malignancies (PGMs). Currently, surgical treatment is the gold standard for resectable tumours and is usually followed by adjuvant radiotherapy (RT) if adverse factors are present, such as advanced tumour stage, nodal involvement, close resection margins, perineural invasion (PNI), lymphovascular invasion (LVI), tumour spillage during surgery, or ACC. Chemotherapy is used together with adjuvant RT if clear margins are not achieved and/or extranodal extension (ENE) is detected in lymph nodes. Surgical planning for these tumours is somewhat controversial, especially regarding the removal of the deep parotid lobe in T1-T2 tumours of the superficial parotid gland and management of a cN0 neck 1.
Furthermore, despite advancements in oncologic research, survival rates of PGMs have remained stable over the last decades. Disease-related deaths occur either from loco-regional failure or development of distant metastasis, even decades after the index treatment. Multiple-site relapses are also described.
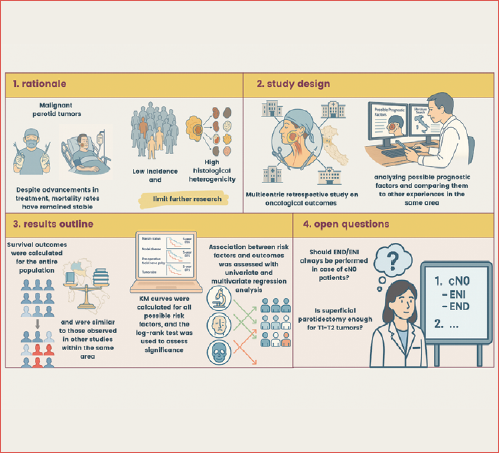
The aim of this retrospective multicentric study is to report the oncologic outcomes of a large cohort of surgically-treated patients affected by PGMs treated at 4 Italian ENT Units. The survival rates and prognostic factors were compared with the experience of other Italian Institutions to highlight similarities and differences in the outcomes of this challenging oncologic disease in the Italian context (Cover figure).
Materials and methods
This is a retrospective multicentric study performed at 4 referral centres for head and neck cancer in Northern Italy. Patients who underwent surgical treatment with curative intent for a PGM between January 2007 and December 2020 at the Otorhinolaryngology - Head and Neck Surgery Department of Bologna, Modena, Verona, and Reggio-Emilia University Hospitals, and at the Maxillo-Facial Surgery Department of Modena University Hospital were considered.
Criteria for inclusion in the study were a histologically proven malignant tumour of the parotid gland and complete availability of medical records. Non-resectable tumours, lymphomas, metastatic tumours at diagnosis, and/or patients with a history of histologically proven squamous cell carcinoma of the skin of the face or the scalp were excluded from the study.
Ultrasonography (US), magnetic resonance imaging (MRI), and computed tomography (CT) were used for preoperative evaluation and staging according to the Eighth Edition of the UICC TNM Classification of Malignant Tumors. Fine needle aspiration cytology (FNAC) was performed in 81.1% of cases.
Head and Neck National Comprehensive Cancer Network (NCCN) guidelines (version 2.2020) and Italian Multidisciplinary guidelines by AIOCC-AIRO-AIOM (2018) were followed for treatment protocol for primary site and neck. Parotid tumours were defined and classified according to the World Health Organization Classification of Tumors (4th Edition, 2017). Surgical margins of 5 mm or more were defined as clear (R0), while margins of 1 to 5 mm were defined as close, although it should be underlined that such a cut-off is amply debated in the literature and there is still not wide consensus on this matter, as recently noted in a systematic review by de Vincentiis et al. 2.
As a secondary endpoint, a review of the Italian literature regarding oncological outcomes of surgically-treated parotid tumours was performed to compare the results of the present study to the current state of the art in Italy. The search was performed on PubMed in June 2024 based on MeSH terms, as follows: [(malignant parotid tumor OR parotid malignancy) AND (surgery OR surgical resection OR parotidectomy) AND (oncologic outcomes OR survival OR locoregional control) AND (Italy OR Italian)]. After running the above search string and duplication removal, the titles and abstracts obtained were screened and full texts were included according to the following inclusion criteria: English, Italian, French or Spanish language; mention of parotid gland malignancies; availability of the full-text. Exclusion criteria were publication year before 2000; case reports, systematic reviews, metanalyses, editorial letters.
The authors extracted data from the articles included using a standardised template and collected in a computerised database. Finally, a qualitative review of the included articles was performed 3-8.
Statistical analysis
Overall survival (OS), disease-free survival (DFS), and disease-specific survival (DSS) proportions at 5 years were calculated according to Kaplan-Meyer curves. Time of observation was calculated as time from the end of treatments to last follow-up for patients who did not experience a recurrence and were alive at the time of last follow-up, while it was calculated as time to recurrence/death for patients who relapsed/died from disease during the follow-up. OS was calculated from the end of treatments to death for any cause.
The comparison between different groups was made with the log-rank test (for dichotomous variables) or the log-rank test for trend (for multiple variables). The Cox proportional hazard model was used for univariate and multivariate analyses. Variables for which convergence was not achieved were excluded from the final Cox regression model.
Patients were divided according to tumour size, parotid lobe involvement, pT category, pN category, final pTNM stage, margin status (R), grading (G), extranodal extension (ENE), histology (the 3 more common ones) and facial nerve involvement. The prognostic impact of these factors was analysed on DSS, instead of OS, due to the low number of deaths by other causes (2 cases).
To assess possible risk factors for nodal metastases, the chi-square test was used for categorical variables, while the t-test was used for continuous variables.
All analyses were performed with GraphPad Prism version 7.0a (GraphPad Software, San Diego CA) and R version 4.2.3 (R Foundation for Statistical Computing©, 2021), with p < 0.05 as the significant cut-off.
Results
General results
A total of 106 patients were eventually included in the study. Mean age of the study cohort was 59 years (range 12-90). The male-to-female ratio was 1:1.26.
Data on clinical and pathological characteristics of enrolled patients are detailed in Table I. The most common histology was MEC (37, 34.9%), followed by AciCC (13, 12.3%) and ACC (12, 11.3%). All other histologies had an absolute count lower than 10 and are detailed in Figure 1.
Parotidectomy I-IV according to the European Salivary Gland Society classification was the most commonly performed procedure (62, 58.5%), followed by parotidectomy I-II (26, 24.5%). Superficial parotidectomy was extended to level III in 12 cases (11.3%), and to level V in 2 cases (1.8%). Partial superficial parotidectomy was performed in the remaining 4 cases (3.7%). Neck dissection (ND) was performed in 34 patients (32.1%), and was always ipsilateral to the side of the primary tumour. Intraoperative frozen sections on level II lymph nodes was performed in 7 cases and was negative in 100% of cases. More than half of patients did not undergo any adjuvant treatment (59, 55.7%), while most of the remaining underwent only adjuvant RT (41 cases, 38.7%).
Follow-up and pattern of tumour recurrence
Median follow-up was 39 months (range 3-110). Patients’ status at last follow-up is reported in Figure 2. Recurrent disease was observed in 15 patients (14.2%). However, for 2, the timing, pattern, and treatment of recurrence was not known and thus excluded. For the remaining 13 patients, mean time to recurrence was 36.2 months (range 6-82). The pattern of recurrence is detailed in Figure 3, with local recurrence in 5 patients (4.7%), regional recurrence in 3 (2.8%) and distant recurrence in 5 (4.7%), of which 2 also had concomitant locoregional recurrence. In 9 cases, salvage surgery was performed, followed by adjuvant RT in 2 patients and by adjuvant CRT in one. Palliative chemotherapy was performed in 2 patients, while best supportive care was indicated in one case.
Survival analysis
Five-year OS, DSS and DFS in the entire study cohort were 84.5%, 83.4% and 82.5%, respectively.
Preoperative facial nerve (FN) palsy did not significantly influence DSS or DFS. Deep lobe involvement, on the other hand, was linked to a significantly lower 5-year DFS compared to involvement of the superficial lobe alone (72 vs 85%, p 0.02). A similar trend was observed for DSS, as patients with lesions extending to the deep lobe had a 5-year DSS of 79% compared to 90% for patients with lesions limited to the superficial lobe (p 0.04).
Tumour size did not affect DFS (p 0.13), but larger dimension was associated with progressively lower 5-year DSS. Specifically, patients with lesions larger than 4 cm had a 5-year DSS of 57% compared to 89% for patients with lesions between 2 and 4 cm, and 93% for patients with lesions smaller than 2 cm (p 0.005).
pT category had an impact on both DFS and DSS. pT1 category was associated with a 5-year DFS of 93% compared to 83% for pT2, 79% for pT3 and 63% for pT4 (p 0.02). Similarly, the 5-year DSS was 100% for pT1, 84% for pT2, and 62% for pT3, while pT4 had a DSS of 71% (p 0.0003).
Nodal disease also greatly influenced recurrence and survival in the study population. Patients with pN0 disease had a 5-year DFS of 100% compared to the 52% for patients with pN+ disease (p 0.004). Similarly, 5-year DSS for pN0 patients was 100% compared to 48% for pN+ patients (p 0.002). ENE+ was associated with a poorer prognosis considering DFS (37.5% vs 86.8% at 5 years, p 0.02), but not DSS (26% vs 83% at 5 years, p 0.06).
Clear surgical margins were associated with a 91% 5-year DFS, compared to 76% for patients with close margins, 84% for patients with microscopically positive margins (R1) and 0% for patients with macroscopically positive margins (R2, p 0.0001). Similarly, R0 was associated with a 96% 5-year DSS vs 83% in case of close margins, 70% in case of R1 and 37% in case of R2 (p 0.0002).
Higher tumour grade was associated with progressively shorter 5-year DFS and DSS. Patients with undifferentiated lesions (G4) had a 5-year DFS of 50% compared to 68% for G3, 75% for G2, and 94% for G1 lesions (p 0.002). Similarly, patients with G3 and G4 lesions had a poorer 5-year DSS (64% and 67%, respectively) with respect to patients with G1 and G2 lesions (91% and 86%, respectively, p 0.004).
Five-year DFS was 100% for AciCC compared to 84.8% for MEC and 67.5% for ACC. This trend was not statistically significant (p = 0.13). Five-year DSS was 100% for AciCC, 86.5% for MEC and 75% for ACC. This trend was not statistically significant at the log-rank for trend test (p = 0.44).
Final TNM stage influenced both recurrence and survival. Stages I and II were associated with better 5-year DFS (96 and 89%, respectively), with respect to Stages III and IV (75 and 64% respectively, p = 0.003). DSS also decreased with increasing Stage (p < 0.0001), with patients affected by a Stage I lesion having a 5-year DSS of 100%, compared to 89% for Stage II, 80% for Stage III and 62% for Stage IV.
Figure 4 and Table II summarise survival analysis with the Kaplan-Meier method.
Subgroup survival analysis
For T1-T2 superficial parotid tumours, R0 was associated with better 5-year DSS (100%), with respect to R close (75%, p = 0.04). In the same group of patients, R0 was associated with a 92.7% 5-year DFS vs 88.9% in case of close margins, but this trend was not statistically significant (p = 0.69).
Parotidectomy extent did not significantly influence DSS or DFS for T1-T2 tumours of the superficial lobe: 5-year DFS was 92.3% for patients subjected to total parotidectomy compared with 100% in patients treated with superficial parotidectomy (p = 0.24), while 5-year DSS was 75% for patients treated with total parotidectomy compared to 100% for patients treated with superficial parotidectomy (p = 0.22).
Similarly, for T3-T4 parotid malignancy, the type of parotidectomy did not have a significant impact on prognosis in terms of DFS and DSS. In detail, 5-year DFS was 67.7% for patients treated with total parotidectomy compared to 72% for patients treated with less-than-total parotidectomy (p = 0.55). Finally, 5-year DSS was 64.4% for patients treated with total parotidectomy compared to 83.3% for patients treated with less-than-total parotidectomy (p = 0.14).
Univariate and multivariate analysis
Factors showing association with DFS in univariate analysis included deep lobe involvement, advanced pT category (pT3-4 vs pT1-2), Stage IV tumours (vs Stage I), positive surgical margins (R1-2 vs R0), histological grade (G2-3 vs G1) and extranodal disease. In multivariate analysis, the only independent prognostic factors for DFS were R2 margin status (vs R0) and G2 histological grade (vs G1).
Regarding DSS, factors showing prognostic value on univariate analysis include > 4 cm size (vs < 2 cm), advanced pT category (pT3-4 vs pT1-2) and R1-R2 margin status (vs R0) (Tab. III). However, no independent prognostic factor for DSS could be identified on multivariate analysis.
Nodal status
Of the 78 cN0 patients, 13 were subjected to elective neck dissection (END). Four of 13 patients showed occult lymph node metastases (30.8%). However, no difference in DFS in cN0 patients undergoing END was seen compared to those who did not (83% vs 84.2%, p > 0.5), as well as in DSS (81% vs 91%, p>0.5) (Figs. 5A-B). Similarly, selecting cN0 patients who were not subjected to END (n = 65), elective neck irradiation (ENI) was not associated with a survival benefit. In fact, DFS at 5 years was 90% for patients undergoing ENI compared to 81.6% for patients not subjected to ENI; however, this trend was not significant at the log-rank test (p 0.72). A similar non-significant trend was observed for 5-year DSS (100% vs 88.3%, p 0.72) (Figs. 5C-D).
Risk factors for nodal metastasis were male gender (p 0.005) and high (G3-G4) grade (p 0.001). Results of chi-square and t-test for all variables are depicted in Table IV.
Adjuvant treatment
Adjuvant treatment (RT or CRT) in pT3-4 patients was shown to improve 5-year DSS (76.9% for patients who received adjuvant treatments vs 41.5% for patients who did not, p 0.047) but did not prove effective in reducing the recurrence rate. The 5-year DFS was 26.7% for patients who did not receive adjuvant treatment compared to 78.1% for patients who did, but this difference was not significant (p 0.12) (Fig. 5E-F).
Literature review
A total of 6 articles 3-8 were included in the qualitative review after screening for exclusion criteria.
Mean 5-year OS in the studies included was 72.8%, which is slightly lower than in our cohort. Mean 5-year DSS in the studies included was 79.6%, and slightly lower than in our cohort. However, median follow-up in our cohort was shorter (39 months) than in the other studies 3-8 (mean 66 months) (Tab. V).
Preoperative FN palsy was found to influence OS and DFS in 2 studies 3,7 and DSS in one 7, while no influence on oncologic outcomes was found in one study 6, similarly to ours. Deep lobe involvement was found to influence DSS in one study 8, apart from ours, where it also correlated with DFS. The other 5 studies 3-7 did not evaluate the influence of this parameter on survival. Tumour size was found to influence DSS in one study 8, apart from ours. pT and pN were shown to correlate with OS in 3 studies 3,5,7, differently from what we observed in our cohort; both parameters correlated with DSS in 3 studies 6-8, apart from ours, and with DFS in 2 studies 3,7, apart from ours. The influence of positive surgical margins on survival was only investigated in 2 3,7, one of which showed an influence of this parameter on OS and DFS. Influence of tumour grade on survival was assessed in a single study 6, which showed a correlation with DSS, similarly to what we observed (Tab. V).
Discussion
This retrospective multicentric study reports oncological outcomes of a large cohort of patients with PGMs treated in 4 Northern Italian referral centres for head and neck cancer across a 13-year timespan.
Regarding epidemiological data, while PGMs more frequently involve males according to the literature, in our series approximately 53% of patients were females. Mean age in our cohort was 59 years, in accordance with previously reported data. In fact, the higher incidence of cases is usually found during the fifth to sixth decade of life. These lesions usually present as a rapidly growing lump in the parotid region. FN palsy is considered a clinical sign pointing to malignancy. In our series, the rate of neoplastic FN palsy was 15%, similar to what has been previously reported in the literature (12-19%). Previous reports have shown that FN palsy at presentation is associated with poorer prognosis 9, probably being a sign of neurotropism. However, in our series, no significant differences were observed in 5-year DFS and DSS comparing patients with FN palsy at presentation to those without.
The observed rate of lymph node metastasis at presentation varies from 18% to 28% depending on the study. In our series, approximately 12% of patients presented with node positive disease.
Even in the modern oncologic era, surgical treatment remains the gold standard upfront therapeutic approach for these lesions. In the present series, where only patients surgically treated with curative intent were included, overall prognosis is good (OS 84.5% and DFS 82.5%), and even slightly higher than previously reported in large international series 10,11, and in comparison to other series from our country 3,5-8, even though unfortunately our median follow-up is shorter than that of other studies. The distribution of prognostic factors in the present cohort should be considered in the interpretation of these favourable outcomes.
In our series, the most frequently encountered subtypes were MEC, followed by AciCC and ACC, which appears to be consistent with other studies on the subject 11. There was a trend for increasingly better prognosis going from AciCC to MEC to ACC, which was however not statistically significant. AciCC was shown to be associated with the best prognosis among other histological subtypes in other series 7,12 followed by MEC and ACC 7. On the other hand, adenocarcinoma and undifferentiated carcinoma have been shown to have the worst outcomes 12.
Interestingly, others have shown that histology has no significant influence on prognosis by itself. Van der Schroeff et al. observed that a prognostic model without histology had similar predictive power as one including it 13. In addition, histology is not included in the validated prognostic index by Vander Poorten et al. 10. Most likely, since the same histological subtype may present in various differentiation states, grade rather than histology should be taken into account when investigating prognosis of PGMs.
In our series, grade was found to be an independent prognostic factor for DFS at multivariate analysis, similar to other studies 3,11.
Other reported prognostic factors include pT and pN classification, stage and margin status 3. In our series, we only observed margin status to be an independent prognostic factor for DFS, apart from histological grade. No significant results were obtained at multivariate analysis regarding the impact of said factors on DSS.
When considering only T1-T2 superficial parotid tumours, clear surgical margins seem to be associated with better 5-year DSS compared to close margins. Park et al. did not find any significant difference in disease recurrence or mortality rates between patients with a safety margin of > 5 mm vs 1-5 mm vs < 1 mm for T1-T2 low grade parotid gland cancer 14. We ascribe this discrepancy to the fact that we did not consider, for this analysis, only low-grade cancers, due to our small sample size.
As previously mentioned, there is no doubt that surgical treatment is the gold standard approach in management of PGMs with curative intent. However, while there is consensus on surgical management for Stage III and IV parotid cancers, in which a total parotidectomy is always deemed necessary, treatment for Stage I and II parotid malignancies poses a problem. Some researchers believe that parotidectomy I-II, or even less than superficial parotidectomy, is the best option for Stage I and II low-grade parotid gland superficial tumours, because it carries a lower risk of FN damage and does not compromise oncological results 15. Others recommend total parotidectomy for all patients with T1-T2 superficial parotid carcinomas, with the strongest argument being the presence of lymph nodes in both parotid gland lobes and their connection to the cervical lymphatic network 16. The embryologic development of the neck lymphatic system is assumed to occur following the incapsulation of the submandibular and sublingual glands, but before the incapsulation of the parotid gland. This is the reason why the parotid gland also contains intra-glandular lymph nodes, differently from the submandibular and sublingual glands. Several authors investigated the distribution of lymph nodes within the parotid gland, demonstrating that the lymphatic presence in the deep lobe is not negligible 17. Nevertheless, no survival benefit has been observed in removing the deep lobe for T1 and T2 superficial parotid tumours, until now. In our series, extension of surgery to the deep lobe for T1 and T2 superficial parotid tumours did not significantly improve DSS or DFS, suggesting that removal of deep parotid lobe could be, in these lesions, not always necessary. Further studies are needed to investigate the prognostic impact of removing the deep parotid lobe in a subgroup of Stage I and II parotid cancers with high risk for occult cervical nodal metastasis. In addition, due to the small sample size we could not differentiate this group of patients according to histological grade.
In our series we failed to demonstrate that, for T3 and T4 parotid malignancies, total parotidectomy is superior to more conservative parotid surgery, probably because of the small sample size.
Regarding the management of the neck in PGMs, while there is consensus, in case of cervical lymph nodes involvement, on the necessity of radical or modified radical ipsilateral neck dissection, followed by adjuvant radiotherapy 1, indications for END in parotid gland malignancies are not standardised among clinicians. Some researchers recommend END for all patients with parotid carcinomas, while others only recommend END for patients with either high-grade lesions or specific histological subtypes 18. In our opinion, the confusion stems from the highly variable rate of occult lymph node metastasis reported in the literature, from 0 to 49% 19, even if recent data from a meta-analysis 20 and 2 systematic reviews with meta-analysis 21,22 narrowed the range to 22-36%. This still wide range may be determined by different proportions of histological subtypes and disease stages in single series 19.
In our cohort, almost 31% of patients had clinically occult cervical metastases, although occult nodal metastases were not found to have a prognostic role, probably due to the small sample size. A multicentric study by Fussey and colleagues showed that older age, high-grade and more advanced primary tumours were associated with higher rates of occult node metastasis 23. Grasl et al. also observed that the risk of occult nodal metastasis was significantly associated with grading in a series of patients with MEC 24, even though the possibility of cervical occult nodal metastasis in low grade or low stage parotid tumours is not negligible 1. In addition, according to a large population-based study by Xiao et al. 25, the incidence of occult metastasis to the neck was highest in salivary duct carcinoma (23.6%), followed by adenocarcinoma NOS (19.9%), carcinoma ex pleomorphic adenoma (11.8%), MEC (9.3%), ACC (7%), basal cell adenocarcinoma (6.3%), AciCC (4.4%), and epithelial-myoepithelial carcinoma (1.5%). In our cohort, out of 4 cN0 pN+ cases, 2 were MECs, one a carcinosarcoma, and one a lympho-epithelial carcinoma. All were graded G3 according to the histopathological report. In addition, we observed an association between the presence of nodal metastases with high grade (including G3 and G4) and male gender. Relevantly, tumour grading, definitive histology and pathologic stage of the parotid primary, which are the most relevant predictors of occult nodal metastasis, are known before surgery in only a limited number of cases. Interestingly, END was not associated with a survival advantage in terms of DFS nor DSS in our cohort. Reviewing the literature, no strong evidence in favour of END can be found.
Alternative approaches for the management of cN0 patients have been suggested across the literature. For instance, Lombardi et al. suggested performing a super-selective (levels I-II) or selective (I-III) neck dissection with frozen sections in cases of high-risk occult nodal disease that could be extended to a comprehensive neck dissection if the nodal disease is confirmed intraoperatively 1. In our series, frozen sections on level II lymph nodes were performed in only 7 cases and was always negative.
Secondly, ENI has been proposed, with promising results, for the management of cN0 cases in patients with high-risk histological features discovered only at definitive exam 26; it could be an alternative to END even in patients who have high-risk of occult nodal metastasis known before surgery, especially when there is a high chance of performing adjuvant RT on the primary tumour 27. However, in our series, no survival benefit was observed in cN0 patients undergoing adjuvant RT on the neck as well as on the primary tumour site in terms of both DFS and DSS.
In our series, ENE+ was associated with a poorer prognosis in terms of DFS, although it did not maintain statistical significance on multivariate analysis. Despite the fact that extranodal extension has been generally considered a relevant prognostic predictor in head and neck tumours and that it has been found a relevant node-related prognosticator for salivary gland cancer by some authors 28, data from other series are somewhat conflicting. For instance Aro et al. and Lombardi et al. demonstrated that ENE did not have impact on survival 29,30. Furthermore, Lombardi et al. proposed 3 revised N-classifications to describe the burden of nodal involvement, none of which considered ENE; each of these were found to be better in OS stratification compared to the 8th Edition of the TNM classification, which considers ENE. This was later on externally validated in a further multicentric cohort 31 and has been recently accepted as the new N grading system for parotid malignancies in the latest 9th TNM Edition.
Finally, adjuvant treatment in parotid gland malignancies is usually recommended for advanced-stage disease (III-IV), intermediate- or high-grade tumours, close or positive margins, lymph node metastases, bone invasion, and perineural and lymphovascular invasion. In our series adjuvant treatment (RT or CRT) was shown to improve 5-year DSS in pT3-T4 patients. Regarding the difference in 5-year DFS, although it appears to be clinically relevant (26.7 vs 78.1%), it was not statistically significant at the log-rank test. The lack of statistical significance may be attributed to the limited number of events and high censoring rate, which weaken the reliability of formal comparisons. This underscores the need for further validation.
Additional limitations of this study include its retrospective nature and sample heterogeneity, which did not allow us to take histology and grading into consideration when performing subgroup analyses. In addition, we were not able to retrieve data on the presence of intraparotid nodal metastasis and on the number of positive cervical lymph node metastases, which would have been useful to fully evaluate the impact of nodal status on survival.
Conclusions
In this retrospective study we investigated prognostic factors for malignant parotid tumors in a multricentic setting, comparing them to the experience of other Italian Institutions and highlighting current controversies. We were able to confirm that tumour grade and margin status are pivotal prognostic factors for DFS. Future research is needed to understand the impact of residual intraparotid lymph nodes on risk of recurrence, and therefore how the deep parotid lobe in T1-T2 superficial parotid tumours should be managed. Nonetheless, we were able to demonstrate that removal of the deep parotid lobe is not always necessary. Similarly, it is still unclear in which subgroup of patients END should be performed.
Conflict of interest statement
The authors declare no conflict of interest.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author contributions
GM: ideated the manuscript; CDG, CC: analysed the data; CC: wrote the manuscript with support from FS, GM. FM, ALM, CV, PR, DM, MDB, RN, CC; retrieved data and build the database, with support from CBFMa, DM, AG, LC, PFN, GM, LP; verified the analytical methods and the findings of this work; MAC: supervised the project. All authors discussed the results and contributed to the final manuscript.
Ethical consideration
This study was approved by the Local Institutional Research Committees (CE-AVEN Emilia Romagna: 0000872/22).
The research was conducted ethically, with all study procedures being performed in accordance with the requirements of the World Medical Association’s Declaration of Helsinki.
Written informed consent was obtained from each participant/patient for study participation and data publication.
History
Received: March 27, 2025
Accepted: July 22, 2025
Figures and tables
Figure 1. Histologies with an absolute count lower than 10 in this cohort. PLGA: polymorphous low grade adenocarcinoma; adenocarcinoma NOS: adenocarcinoma not otherwise specified; carcinoma ex-PA: carcinoma ex-pleomorphic adenoma.
Figure 2. Patients’ status at last follow-up. NED: no evidence of disease; AWD: alive with disease; DWD: died with disease; DOD: died of other disease.
Figure 3. Pattern of recurrence.
Figure 4. Survival analysis with the Kaplan-Meier method. DSS: disease-specific survival; DFS: disease-free survival; FN: facial nerve; < 2 cm: tumour size smaller than 2 cm; 2-4 cm: tumour size between 2 and 4 cm; > 4 cm: tumour size larger than 4 cm; pN0: no evidence of cervical lymph node metastases on the pathological report; pN+: pathologically-proven cervical lymph node metastases; ENE: extra nodal extension; MEC: mucoepidermoid carcinoma; AciCC: acinic cell carcinoma; ACC: adenoid cystic carcinoma; I: Stage I; II: Stage II; III: Stage III; IV: Stage IV.
Figure 5. Impact of treatment with the Kaplan-Meier method. DSS: disease-specific survival; DFS: disease-free survival; END: elective neck dissection; ENI: elective neck irradiation; RT: adjuvant treatment.
| N (%) | ||
|---|---|---|
| Male | 47 (44.3) | |
| Preoperative FN palsy | 16 (15.1) | |
| Clinical T category | cT1 | 36(34) |
| cT2 | 38 (35.8) | |
| cT3 | 4 (3.7) | |
| cT4a | 11 (10.4) | |
| cT4b | 1 (0.9) | |
| NA | 16 (15.1) | |
| Clinical N category | cN0 | 78 (73.6) |
| cN+ | 13 (12.3) | |
| NA | 15 (14.2) | |
| Size (cm) | < 2 | 43 (40.6) |
| 2-4 | 45 (42.5) | |
| > 4 | 17(16) | |
| NA | 1 (0.9) | |
| Deep lobe involvement | 48 (45.3) | |
| Histology | MEC | 37 (34.9) |
| AciCC | 13 (12.3) | |
| ACC | 12 (11.3) | |
| Other | 44 (41.5) | |
| ND | 34 (32.1) | |
| Pathological T category | pT1 | 35(33) |
| pT2 | 31 (29.2) | |
| pT3 | 16 (15.1) | |
| pT4 | 23 (21.7) | |
| NA | 1 (0.9) | |
| Histological grade | 1 | 46 (43.4) |
| 2 | 18(17) | |
| 3 | 28 (26.4) | |
| Undifferentiated | 3 (2.8) | |
| NA | 11 (10.4) | |
| Margin status | R0 | 58 (54.7) |
| R close | 19 (17.9) | |
| R1 | 25 (23.6) | |
| R2 | 4 (3.7) | |
| Pathological N+ | 16 (47.1)* | |
| ENE+ | 8(50)** | |
| Pathological TNM stage | I | 32 (30.2) |
| II | 29 (27.4) | |
| III | 14 (13.2) | |
| IV | 30 (28.3) | |
| NA | 1 (0.9) | |
| Adjuvant treatments | None | 59 (55.7) |
| RT | 41 (38.7) | |
| CRT | 5 (4.7) | |
| NA | 1 (0.9) | |
| * Percent of pN+ cases was calculated on the total number of cases subjected to neck dissection; **Percent of ENE+ cases was calculated on total number of pN+ cases. Histologies different from MEC, AciCC and ACC all had an absolute count lower than 10 in this cohort; FN: facial nerve; MEC: mucoepidermoid carcinoma; AciCC: acinic cell carcinoma; ACC: adenoidocistic carcinoma; ND: neck dissection; ENE: extranodal extension; RT: radiotherapy; CRT: chemoradiation; NA: not available. | ||
| 5-year DFS (%) | p | 5-year DSS (%) | p | ||
|---|---|---|---|---|---|
| Size (cm) | < 2 | 88.9 | 0.1340 | 93.6 | 0.005* |
| 2-4 | 77.1 | 88.6 | |||
| > 4 | 60.9 | 56.8 | |||
| Lobe involved | Superficial | 85.4 | 0.0236* | 90 | 0.0377* |
| Deep | 72.3 | 79.5 | |||
| Pathological T category | 1 | 92.9 | 0.0209* | 100 | 0.0003* |
| 2 | 83.2 | 84.1 | |||
| 3 | 79.1 | 61.5 | |||
| 4 | 63.3 | 71.1 | |||
| Pathological nodal status | Negative | 100 | 0.004* | 100 | 0.0019* |
| Positive | 52 | 47.5 | |||
| Pathological TNM stage | I | 96.1 | 0.0035* | 100 | < 0.0001* |
| II | 89 | 88.8 | |||
| III | 74.5 | 80 | |||
| IV | 64.5 | 62.2 | |||
| Margin status | R0 | 91.3 | 0.0001* | 95.9 | 0.0002* |
| R close | 76.5 | 82.8 | |||
| R1 | 84.2 | 70.1 | |||
| R2 | 0 | 37.5 | |||
| Histological grade | 1 | 94.1 | 0.0024* | 90.6 | 0.0036* |
| 2 | 75.1 | 85.7 | |||
| 3 | 67.6 | 64.2 | |||
| Undifferentiated | 50 | 66.6 | |||
| ENE | Negative | 86.8 | 0.0171* | 83 | 0.0587 |
| Positive | 37.5 | 25.7 | |||
| Histology | AciCC | 100 | 0.1266 | 100 | 0.4431 |
| MEC | 84.7 | 86.5 | |||
| ACC | 67.5 | 75 | |||
| Facial nerve | No palsy | 83.9 | 0.1255 | 86.4 | 0.0857 |
| Palsy | 72.7 | 80.2 | |||
| MEC: mucoepidermoid carcinoma; AciCC: acinic cell carcinoma; ACC: adenoidocistic carcinoma; ENE: extranodal extension. * p < 0.05. | |||||
| Univariate analysis | ||||||
|---|---|---|---|---|---|---|
| coef | exp(coef) | se(coef) | z | p | ||
| Disease-free survival | ||||||
| Size (cm)n = 102, number of events = 15 | < 2 (ref) | |||||
| 2-4 | 0.3934 | 1.4821 | 0.6081 | 0.647 | 0.518 | |
| > 4 | 1.0082 | 2.7406 | 0.6729 | 1.498 | 0.134 | |
| Lobe involvedn = 103, number of events = 15 | Superficial (ref) | |||||
| Deep | 1.2479 | 3.4829 | 0.5868 | 2.127 | 0.0335* | |
| Pathological T categoryn = 103, number of events = 15 | 1 (ref) | |||||
| 2 | 0.9190 | 2.5068 | 0.9176 | 1.002 | 0.3166 | |
| 3 | 1.3863 | 4.0002 | 0.9159 | 1.514 | 0.1301 | |
| 4 | 1.8954 | 6.6554 | 0.8040 | 2.357 | 0.0184* | |
| Pathological TNM stagen = 102, number of events = 15 | I (ref) | |||||
| II | 0.9947 | 2.7038 | 1.2266 | 0.811 | 0.4174 | |
| III | 1.8586 | 6.4149 | 1.2301 | 1.511 | 0.1308 | |
| IV | 2.3966 | 10.9854 | 1.0505 | 2.281 | 0.0225* | |
| Margin statusn = 103, number of events = 15 | R0 (ref) | |||||
| R close | 0.7878 | 2.1985 | 0.7692 | 1.024 | 0.3057 | |
| R1 | 1.4008 | 4.0583 | 0.6742 | 2.078 | 0.0377* | |
| R2 | 3.3479 | 28.4439 | 0.8074 | 4.146 | 0.005 | |
| Histological graden = 92, number of events = 13 | 1 (ref) | |||||
| 2 | 2.418 | 11.226 | 1.119 | 2.161 | 0.0307* | |
| 3 | 2.626 | 13.813 | 1.071 | 2.453 | 0.0142* | |
| Undifferentiated | 2.457 | 11.673 | 1.418 | 1.733 | 0.0831 | |
| ENE n = 16, number of events = 7 | Negative (ref) | |||||
| Positive | 0.9467 | 2.5772 | 0.8451 | 1.12 | 0.263 | |
| Disease-specific survival | ||||||
| Size (cm)n = 103, number of events = 12 | < 2 (ref) | |||||
| 2-4 | 1.1080 | 3.0282 | 0.8385 | 1.321 | 0.1863 | |
| > 4 | 2.1068 | 8.2219 | 0.8377 | 2.515 | 0.0119* | |
| Lobe involvedn = 104, number of events = 12 | Superficial (ref) | |||||
| Deep | 1.2988 | 3.6647 | 0.6688 | 1.942 | 0.0522 | |
| Pathological T categoryn = 104, number of events = 12 | 1-2 (ref) | |||||
| 3-4 | 2.2527 | 9.5131 | 0.7753 | 2.906 | 0.00367* | |
| Margin statusn = 104, number of events = 12 | R0 (ref) | |||||
| R close | 1.0152 | 2.7599 | 1.0020 | 1.013 | 0.31098 | |
| R1 | 2.1236 | 8.3613 | 0.8177 | 2.597 | 0.00940* | |
| R2 | 3.0198 | 20.4863 | 1.0111 | 2.986 | 0.00282* | |
| ENEn = 38, number of events = 9 | Negative (ref) | |||||
| Positive | 1.3501 | 3.8578 | 0.7682 | 1.757 | 0.0788 | |
| Facial nerve n = 104, number of events = 12 | No palsy (ref) | |||||
| Palsy | 1.0100 | 2.7455 | 0.6129 | 1.648 | 0.0994 | |
| Multivariate analysis | ||||||
| coef | exp(coef) | se(coef) | z | p | ||
| Disease-free survival | ||||||
| Lobe involvedn = 91, number of events = 13 | Superficial (ref) | |||||
| Deep | 1.2892 | 3.6297 | 0.8286 | 1.556 | 0.1198 | |
| Pathological T categoryn = 91, number of events = 13 | 1-2 (ref) | |||||
| 3-4 | -0.4531 | 0.6356 | 0.8935 | -0.507 | 0.6121 | |
| Margin statusn = 103, number of events = 15 | R0 (ref) | |||||
| R close | 0.7161 | 2.0464 | 0.9345 | 0.766 | 0.4435 | |
| R1 | 1.0722 | 2.9219 | 0.9066 | 1.183 | 0.2369 | |
| R2 | 3.0094 | 20.2753 | 1.2282 | 2.450 | 0.0143* | |
| Histological graden = 92, number of events = 13 | 1 (ref) | |||||
| 2 | 2.4025 | 11.0504 | 1.1737 | 2.047 | 0.0407* | |
| 3 | 2.2747 | 9.7248 | 1.1940 | 1.905 | 0.0568 | |
| Undifferentiated | 2.5092 | 12.2949 | 1.4567 | 1.723 | 0.0850 | |
| Disease-specific survival | ||||||
| n = 103, number of events = 12 | ||||||
| Size (cm) | < 2 (ref) | |||||
| 2-4 | 0.4936 | 1.6381 | 0.8729 | 0.565 | 0.5718 | |
| > 4 | 1.0897 | 2.9735 | 0.8890 | 1.226 | 0.2203 | |
| Pathological T category | 1-2 (ref) | |||||
| 3-4 | 1.3198 | 3.7428 | 0.8744 | 1.509 | 0.1312 | |
| Margin status | R0 (ref) | |||||
| R close | 0.7176 | 2.0496 | 1.0265 | 0.699 | 0.4845 | |
| R1 | 1.5344 | 4.6387 | 0.8594 | 1.786 | 0.0742 | |
| R2 | 1.9252 | 6.8569 | 1.0773 | 1.787 | 0.0739 | |
| ENE: extra nodal extension. *p < 0.05. | ||||||
| pN0 (%) | pN+ (%) | p | ||
|---|---|---|---|---|
| Gender | Male | 18.2 | 81.8 | 0.005* |
| Female | 69.6 | 30.4 | ||
| Facial nerve | No palsy | 56 | 44 | 0.551 |
| Palsy | 44.4 | 55.6% | ||
| Histology | MEC | 57.1 | 42.9 | 0.159 |
| AciCC | 100 | 0 | ||
| ACC | 100 | 0 | ||
| Lobe involved | Superficial | 69.2 | 30.8 | 0.134 |
| Deep | 42.9 | 57.1 | ||
| Size (cm) | < 2 | 70 | 30 | 0.412 |
| 2-4 | 42.9 | 57.1 | ||
| > 4cm | 50 | 50 | ||
| Histological grade | 1 | 90 | 10 | 0.001* |
| 2 | 100 | 0 | ||
| 3 + 4 (high grade) | 25 | 75 | ||
| Pathological T stage | 1 | 75 | 25 | 0.198 |
| 2 | 71.4 | 28.6 | ||
| 3 | 42.9 | 57.1 | ||
| 4 | 33.3 | 66.7 | ||
| Age (mean, SD) | 60.4, 12.9 | 65.3, 13.1 | ||
| MEC: mucoepidermoid carcinoma; AciCC: acinic cell carcinoma; ACC: adenoid cystic carcinoma; pN0: no evidence of cervical lymph node metastases on the pathological report; pN+: pathologically-demonstrated cervical lymph node metastases. * p value < 0.05. | ||||
| Authors (year of publication) | Nagliati et al. 5 | Mercante et al. 6 | Paderno et al. 7 | Molteni et al. 8 | Mannelli et al. 3 | Varazzani et al. 4 | Present paper |
|---|---|---|---|---|---|---|---|
| Institution(s) | Trieste | Roma | Brescia | Modena | Firenze | Parma | Multicentric |
| No. of surgically treated patients | 104 | 141 | 104 | 74 | 219 | 48 | 106 |
| Prognostic factors | |||||||
| Preop facial nerve palsy | NA | ns | OS-DSS-DFS | NA | OS-DFS | NA | ns |
| Deep lobe involvement | NA | NA | NA | DSS | NA | NA | DSS-DFS |
| Tumour size | NA | NA | NA | DSS | NA | NA | DSS |
| pT | OS | DSS | OS-DSS-DFS | DSS | OS-DFS | NA | DSS-DFS |
| pN | OS | DSS | OS-DSS-DFS | DSS | OS-DFS | NA | DSS-DFS |
| Positive surgical margins | NA | NA | ns | NA | OS-DFS | NA | DSS-DFS |
| Histology | ns | ns | OS-DSS-DFS | DSS | OS-DFS | NA | ns |
| Grading | NA | DSS | NA | NA | NA | NA | DSS-DFS |
| TNM stage | NA | OS-DSS | OS-DSS-DFS | DSS | OS -DFS | NA | DSS-DFS |
| 5-y OS (%) | 58 | 72.3 | 74.7 | 77.4 | 68.7 | 85.4 | 84.5 |
| 5-y DSS (%) | 78 | 75 | 80.4 | 77.4 | 73.0 | 93.7 | 83.4 |
| 5-y DFS (%) | 82 | 82.1 (L) | 66.9 | 68.4 | 75.0 (L) | 89.6 | 82.5 |
| 89.5 (D) | 83.2 (R) | ||||||
| Median follow-up in months (range) | 47 | 69 | 51 | 51 | 95 | 84 (mean) | 39 |
| (12-153) | (7-279) | (3-245) | (26-76) | (7-180) | (3-110) | ||
| OS: overall survival; DSS: disease-specific survival; DFS: disease-free survival; L: local; D: distant; R: regional; NA: not available; ns: not significant. | |||||||
References
- Lombardi D, McGurk M, Vander Poorten V. Surgical treatment of salivary malignant tumors. Oral Oncol. 2017;65:102-113. doi:https://doi.org/10.1016/j.oraloncology.2016.12.007
- de Vincentiis M, Pagliuca G, Margani V. Margins in major salivary gland surgery: clinical and pathological criteria for defining margins and their implications on the choice of multimodal therapies. A systematic review. Acta Otorhinolaryngol Ital. 2025;45:S109-S120. doi:https://doi.org/10.14639/0392-100X-suppl.1-45-2025-N1108
- Mannelli G, Alessandro F, Martina F. Nomograms predictive for oncological outcomes in malignant parotid tumours: recurrence and mortality rates of 228 patients from a single institution. Eur Arch Otorhinolaryngol. 2022;279:4491-4503. doi:https://doi.org/10.1007/s00405-019-05556-9
- Varazzani A, Tognin L, Bergonzani M. Diagnosis and management of parotid gland cancer with focus on the role of preoperative fine-needle aspiration cytology: a 10-year-long retrospective study with 5-year follow-up. J Maxillofac Oral Surg. 2023;22:373-380. doi:https://doi.org/10.1007/s12663-023-01849-z
- Nagliati M, Bolner A, Vanoni V. Surgery and radiotherapy in the treatment of malignant parotid tumors: a retrospective multicenter study. Tumori J. 2009;95:442-448. doi:https://doi.org/10.1177/030089160909500406
- Mercante G, Marchese C, Giannarelli D. Oncological outcome and prognostic factors in malignant parotid tumours. J Craniomaxillofac Surg. 2014;42:59-65. doi:https://doi.org/10.1016/j.jcms.2013.02.003
- Paderno A, Tomasoni M, Mattavelli D. Primary parotid carcinoma: analysis of risk factors and validation of a prognostic index. Eur Arch Otorhinolaryngol. 2018;275:2829-2841. doi:https://doi.org/10.1007/s00405-018-5122-1
- Molteni G, Molinari G, Ghirelli M. Oncological outcomes of parotid gland malignancies: a retrospective analysis of 74 patients. J Stomatol Oral Maxillofac Surg. 2019;120:310-316. doi:https://doi.org/10.1016/j.jormas.2019.03.006
- Terakedis B, Hunt J, Buchmann L. The prognostic significance of facial nerve involvement in carcinomas of the parotid gland. Am J Clin Oncol. 2017;40:323-328. doi:https://doi.org/10.1097/COC.0000000000000157
- Poorten V, Hart A, Vauterin T. Prognostic index for patients with parotid carcinoma: international external validation in a Belgian-German database. Cancer. 2009;115:540-550. doi:https://doi.org/10.1002/cncr.24015
- Kim Y, Chung W, Jeong J. Evaluation of prognostic factors for the parotid cancer treated with surgery and postoperative radiotherapy. Clin Exp Otorhinolaryngol. 2020;13:69-76. doi:https://doi.org/10.21053/ceo.2019.00388
- Wahlberg P, Anderson H, Biörklund A. Carcinoma of the parotid and submandibular glands – A study of survival in 2465 patients. Oral Oncol. 2002;38:706-713. doi:https://doi.org/10.1016/s1368-8375(02)00007-6
- van der Schroeff M, Terhaard C, Wieringa M. Cytology and histology have limited added value in prognostic models for salivary gland carcinomas. Oral Oncol. 2010;46:662-666. doi:https://doi.org/10.1016/j.oraloncology.2010.06.007
- Park Y, Kang M, Kim D. Surgical extent and role of adjuvant radiotherapy of surgically resectable, low-grade parotid cancer. Oral Oncol. 2020;107. doi:https://doi.org/10.1016/j.oraloncology.2020.104780
- Lim Y, Lee S, Kim K. Conservative parotidectomy for the treatment of parotid cancers. Oral Oncol. 2005;41:1021-1027. doi:https://doi.org/10.1016/j.oraloncology.2005.06.004
- Olsen K, Moore E. Deep lobe parotidectomy: clinical rationale in the management of primary and metastatic cancer. Eur Arch Otorhinolaryngol. 2014;271:1181-1185. doi:https://doi.org/10.1007/s00405-013-2616-8
- Sönmez S, Orhan K, Kara E. Determining the number and distribution of intraparotid lymph nodes according to parotidectomy classification of European Salivary Gland Society: cadaveric study. Head Neck. 2020;42:3685-3692. doi:https://doi.org/10.1002/hed.26434
- Kaura A, Kennedy R, Ali S. Utility of neck dissection for management of carcinoma of the parotid gland. Br J Oral Maxillofac Surg. 2019;57:1039-1043. doi:https://doi.org/10.1016/j.bjoms.2019.09.002
- Ng-Cheng-Hin B, Glaholm J, Awad Z. Elective management of the neck in parotid tumours. Clin Oncol R Coll Radiol GB. 2018;30:764-772. doi:https://doi.org/10.1016/j.clon.2018.08.017
- Warshavsky A, Rosen R, Muhanna N. Rate of occult neck nodal metastasis in parotid cancer: a meta-analysis. Ann Surg Oncol. 2021;28:3664-3671. doi:https://doi.org/10.1245/s10434-020-09331-7
- Ho J, Mair M, Noor A. Systematic review and meta-analysis on the incidence of level-specific cervical nodal metastasis in primary parotid malignancies. Otolaryngol Head Neck Surg. 2023;168:1279-1288. doi:https://doi.org/10.1002/ohn.207
- Borsetto D, Iocca O, De Virgilio A. Elective neck dissection in primary parotid carcinomas: a systematic review and meta-analysis. J Oral Pathol Med. 2021;50:136-144. doi:https://doi.org/10.1111/jop.13137
- Fussey J, Tomasoni M, Tirelli G. Prognostic indicators in clinically node-negative malignant primary salivary tumours of the parotid: a multicentre experience. Oral Oncol. 2021;123. doi:https://doi.org/10.1016/j.oraloncology.2021.105577
- Grasl S, Janik S, Faisal M. Influence of grading on management and outcome in mucoepidermoid carcinoma of the parotid - A multi-institutional analysis. Laryngoscope. 2023;133:124-132. doi:https://doi.org/10.1002/lary.30135
- Xiao C, Zhan K, White-Gilbertson S. Predictors of nodal metastasis in parotid malignancies: a national cancer data base study of 22,653 patients. Otolaryngol Head Neck Surg. 2016;154:121-130. doi:https://doi.org/10.1177/0194599815607449
- Park J, Wu H, Kim J. Adjuvant radiotherapy in node-negative salivary malignancies of the parotid gland: a multi-institutional analysis. Radiother Oncol. 2023;183. doi:https://doi.org/10.1016/j.radonc.2023.109554
- Herman M, Werning J, Morris C. Elective neck management for high-grade salivary gland carcinoma. Am J Otolaryngol. 2013;34:205-208. doi:https://doi.org/10.1016/j.amjoto.2012.11.012
- Lee H, Roh J, Cho K. Positive lymph node number and extranodal extension for predicting recurrence and survival in patients with salivary gland cancer. Head Neck. 2020;42:1994-2001. doi:https://doi.org/10.1002/hed.26135
- Aro K, Ho A, Luu M. Development of a novel salivary gland cancer lymph node staging system. Cancer. 2018;124:3171-3180. doi:https://doi.org/10.1002/cncr.31535
- Lombardi D, Tomasoni M, Paderno A. The impact of nodal status in major salivary gland carcinoma: a multicenter experience and proposal of a novel N-classification. Oral Oncol. 2021;112. doi:https://doi.org/10.1016/j.oraloncology.2020.105076
- Lombardi D, Tomasoni M, Missale F. Nodal status in major salivary gland cancer: external validation of a novel N-classification. Eur J Surg Oncol. 2025;51. doi:https://doi.org/10.1016/j.ejso.2025.110006
Downloads
License
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Copyright
Copyright (c) 2026 Società Italiana di Otorinolaringoiatria e chirurgia cervico facciale
How to Cite
- Abstract viewed - 410 times
- PDF downloaded - 94 times




